This article is part 3 of Dr. Glenn Clark’s lecture on Sleep Disordered Breathing for Dental Residents of the Online Master of Science in Orofacial Pain and Oral Medicine program at the Herman Ostrow School of Dentistry of USC.
What is snoring?
Primary snoring is characterized by loud upper-airway breathing sounds in sleep, without episodes of sleep apnea or hypoventilation. The snoring typically occurs while the patient is in the supine position and is usually continuous, present with each breath, and not accompanied by arousals or other evidence of sleep disturbance.
While snoring disorders is generally perceived as a social nuisance, rating of its noisiness is subjective and, therefore, inconsistent. Objective assessment of snoring is important to evaluate the effect of treatment interventions. Moreover, snoring carries information relating to the site and degree of obstruction of the upper airway.
Like what you’re learning? Take it a step further and test your clinical diagnosis skills with USC’s Virtual Patient Simulation. Review real-life patient histories, symptoms, and imaging, conduct a medical interview and clinical exam, make a diagnosis, and create a treatment plan for virtual patients experiencing Orofacial Pain conditions.
Symptoms of Snoring Disorders
The patient occasionally is aware of the snoring, but many snorers swear they do not snore when told about this problem. The patient has no complaint of insomnia or excessive sleepiness. The snoring patient may experience a dry mouth, which can lead to awakenings with a desire to drink water. A flutter of the soft palate accounts for most of louder snoring sounds produced by patients.
Causes of Snoring
Snoring is subject to many influences such as body position, sleep stage, route of breathing, and the presence or absence of sleep-disordered breathing. Its presentation may be variable within or between nights.
Decibel Level of Snoring
A person who snores not only disturbs the sleep of others but if it is loud, they might disturb their sleep. Snoring levels vary between and within a single individual. The mean peak levels of snoring recorded are between 50 and 65 decibels. Snoring could reach high noise-level in the range of 80-90 decibel that matches the decibel levels of a vacuum cleaner. Below is a table to allow the reader to understand noise levels produced by a variety of activities.
Remember: decibels are logarithmic, meaning a 10-point change is a 10-fold increase in the sound.
The loudness of the snoring is not indicative of the severity of obstruction. If the upper airways are tremendously obstructed, there may not be enough air movement to make much sound, and even the loudest snoring doesn’t mean the individual has sleep apnea syndrome.
How prevalent is snoring?
Snoring is a prevalent disorder affecting 20-40% of the general population with 30% of the adult population over the age of 30 snoring, and the prevalence of snoring increasing in both men and women with age. Prevalence of snoring rises to 40% to 50% of men and women over the age of 65 years and then decreases for older individuals. This decrease in snoring of people older than 65-years-old may be due to a reduction in deep NREM and REM sleep that occurs with increasing age.
Types of Snoring Sounds
In a general sense, snoring is the turbulent sound of air moving through the back of the mouth, nose, and throat. However, there are several types of snoring sounds that patients produce. Nasal tissue sounds, palatal flutter sounds, and other sounds.
1. Palatal Flutter Sounds
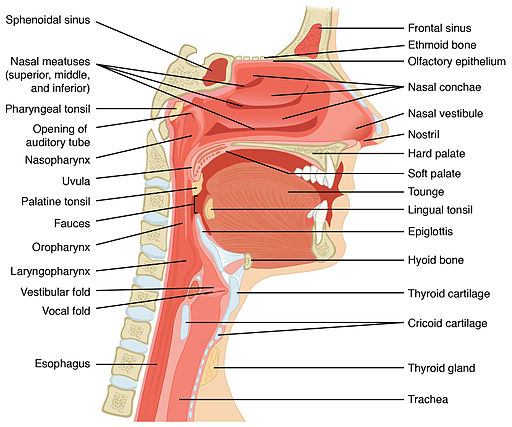
The most common explanation for snoring is the sound usually is produced by the vibration of pharyngeal tissues (posterior base of the tongue, soft palate, uvula, posterior pharyngeal wall) due to turbulent air flow through a narrow oropharyngeal.
It appears that the pitch of the palatal snoring sound is in the low-frequency range (<200 Hz) and its pitch is determined by vibration of the soft palate. Palatal surgery is known to alter the sound characteristics of snoring.
2. Non-Palatal or Nasal Snoring
A much less common form of snoring is non-palatal snoring. One explanation for non-palatal snoring is nasal tissue vibration sound; another is the sound produced in the retroglossal or hypoglossal region of the throat. Specifically sound coming from tissue vibration in the epiglottis, hypopharyngeal, and tongue base area. Regardless of the site of the vibrating tissues, the sound is produced by turbulent air flow through a narrow nasopharyngeal space.
Snoring originating from the nasal passage occurs because the nasal mucous tissues are swollen or there are thick mucus secretions on these tissues that reduce the nasal airway. As air moves through the narrow passage, this causes a vibration of the soft tissues and the mucosal wall surface in the nasal passage to vibrate and create sounds.
When a patient has rhinitis (due to allergies or a cold) and snoring, it is common to put such a patient on nasal steroids to try to reduce the mucosal tissue swelling and secretions, hoping that this will also reduce the snoring, but often without success.
A 2010 study examined the effect of nasal steroids on snoring in patients with rhinitis. This study evaluated an intranasal corticosteroid, fluticasone propionate, in 24 consecutive snorers with associated rhinitis using a randomized, placebo-controlled, crossover design. Patients underwent polysomnography, snoring noise, and nasal airflow resistance (NAR) measurements as a baseline and after each 4-week treatment period.
The results showed that 23 out of 24 subjects completed the study, and of these, 13 were apnea and snoring subjects, and ten were snoring only (non-apnea) subjects. The apnea-hypopnea index for the whole group was significantly lower following treatment with fluticasone than with placebo. Nasal airflow resistance was also considerably lower on fluticasone for the entire group. Unfortunately, snoring noise and sleep quality was unchanged with fluticasone, which suggests that most snoring is not due to nasal congestion but palatal flutter, which is not altered with nasal steroid use.
3. Retroglossal, Epiglottal, and Hypoglossal Snoring
A recent review examined the acoustics of snoring. Among other things, this review speculated that non-palatal snoring is more ‘noise-like,’ and has scattered energy content in the higher spectral sub-bands (>500 Hz). The actual data for this speculation comes for two studies which measured the acoustic characteristics of palatal and non-palatal snoring by acoustic crest factor analysis.
Snoring data were collected from 11 supine adult patients under intravenous sedation (midazolam), using a digital tape recorder. All recordings were analyzed, and the frequency spectrum was determined. The source of the snoring vibration was determined by direct visual confirmation using a nasal endoscope, which was taken as the gold standard.
In six patients, the dominant site was the soft palate. The non-palatal group (five patients) comprised of one epiglottic, two hypopharyngeal, and two tongue base snorers. Based on their analysis, they concluded that palatal snoring produces explosive peaks of sound at low frequency (below approximately 100 Hz). In contrast, non-palatal snorers produced a higher frequency snoring sound.
Another study, by the same authors, examined the assumption that the source of the snoring could be reliably determined by nasal endoscopy. The authors used another group of 5 snoring subjects on whom they performed sleep nasendoscopy, but in this situation, they relied on natural sleep, and they recorded the subjects across the entire night.
Some recordings showed reproducibility, but others showed substantial changes between recordings an hour apart. The authors found that the snoring mechanism may change in some individuals during the night, with or without a change of snore site and that a single drug-induced recording, as in sleep nasendoscopy, was not an adequate method for the diagnosis of the site of snoring. They suggested that the acoustic characteristics might be a better diagnostic method than nasal endoscopy, since in all instances, the frequency of the snoring sound predicted the site of the recording.
What are the risk factors for snoring?
Although not everyone who snores is experiencing difficulty breathing, snoring in combination with other conditions such as overweight and obesity is highly predictive of OSA risk. It is suspected that some patients with primary snoring may be predisposed to developing obstructive sleep apnea syndrome, especially following weight gain or administration of central-nervous-system depressants such as alcohol, anxiolytics, or hypnotics.
Continue your Dental Education Online
Do you want to deliver appropriate and safe care to your growing and ageing dental patients? Consider enrolling in our online, competency-based certificate or Master of Orofacial Pain and Oral Medicine degree programs.