Owing to the increased morbidity of surgery, it is usually reserved as a last resort for those patients that fail to respond to medications or for those that develop resistance to botox injections and there are several methods described in the literature. The surgical management includes ablation techniques (ranging from a myectomy to a pallidotomy), and deep brain stimulation.
Myectomy
The surgical removal of an affected muscle is referred to as myectomy and is usually done for patients with Blepharospasm that fail to respond to conservative management. [1] [2]
Eyelid protractor myectomy provides benefit for patients with essential blepharospasm. [3] A subset of patients with Blepharospasm may not have the actual spasms but experience an “apraxia” of the lid opening also known as “dystonic lid-opening disorder of the levator-inhibiting type”. In these patients, orbicularis spasms are absent and patients try to open their eyes by innervating their frontalis muscle or by using their finger tip.
For ptosis of the eyelids, a viable and less invasive than myectomy alternative is the frontalis sling operation, lifting the upper eyelid to improve esthetics and visual field. [4] [5]
Like what you’re learning? Test your diagnosis skills with USC’s Virtual Patient Simulation. Review real-life patient histories, conduct medical interviews and exams, make a diagnosis, and create a treatment plan for patients experiencing orofacial pain.

Pallidotomy
In patients with oromandibular dystonia, abnormal electrical activity in the external and internal portions of the globus pallidus and the surrounding structures of the basal ganglia has been recorded, therefore, central surgical management (including ablative surgery) has focused on targeting this structure. [6]
Pallidectomy is an invasive procedure that involves creating a surgical lesion in the globus pallidus and may be done unilaterally or bilaterally. Once a popular surgical modality for the management of movement disorders, pallidotomy is not so widely used nowadays due to the invasiveness of the procedure and associated surgical risks. [7] [8]
Deep Brain Stimulation (DBS)
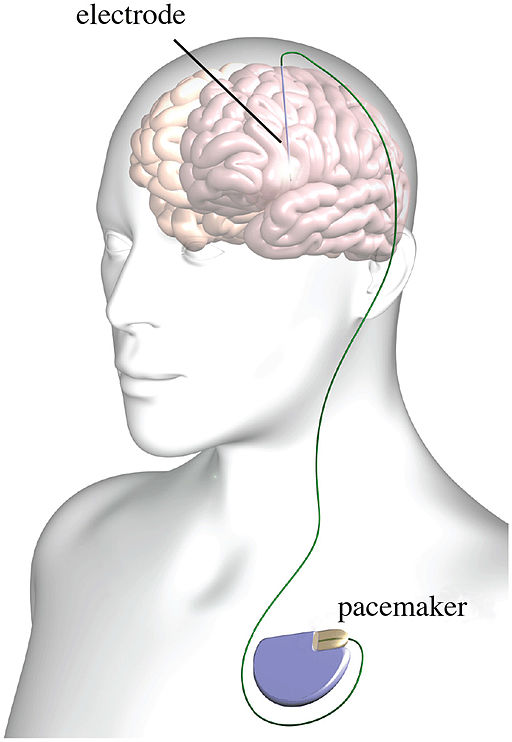
Unlike ablative surgery, such as thalamotomy and pallidotomy, deep brain stimulation (DBS) is reversible and adjustable, thus offering a viable alternative for patients with disabling dystonia. [9]
An implanted electrode to deliver continuous high-frequency electrical stimulation to the thalamus, globus pallidus, or any part of the brain that is involved with the control of movement. [10]
Vidailhet et al [11] reported on the quality of life after bilateral deep brain stimulation of the globus pallidus in 22 patients with generalized dystonia. A 16% increase in the general health, 21% increase in physical function and 10% increase in vitality were observed, with no changes in mood or cognition at the end of 12 months following onset of DBS.
Some data indicates that in patients with Tourette’s syndrome and Parkinson’s disease the modulation of the thalamic driven movements and motor symptoms will be reduced with deep brain stimulation, by altering the basal ganglia-thalamo-cortical circuit. [12] [13]
Although the results of DBS seem very promising, further studies are required to determine the long-term efficacy of this technique.
Previous Articles on Treating Oromandibular Dystonia
Don’t forget to check out our previous articles on treating Oromandibular Dystonia:
- Treating Oromandibular Dystonia: Sensory Tricks & Medical Management
- Chemodenervation Injections for Treating Oromandibular Dystonia
Earn an Online Postgraduate Degree in Orofacial Pain and Oral Medicine
Are you interested in a variety of issues focused on orofacial pain, medicine and sleep disorders? Consider enrolling in the Herman Ostrow School of Dentistry of USC’s online, competency-based certificate or master’s program in Orofacial Pain and Oral Medicine.
References
[1] Green, K., Rastall, D., & Eggenberger, E. (2017). Treatment of Blepharospasm/Hemifacial Spasm. Current Treatment Options in Neurology, 19( 11), 41.
[2] Pariseau, B., Worley, M., & Anderson, R. (2013). Myectomy for blepharospasm 2013. Current Opinion in Ophthalmology, 24(5), 488-493.
[3] Clark, J., Randolph, J., Sokol, J., Moore, N., Lee, H., & Nunery, W. (2017). Surgical approach to limiting skin contracture following protractor myectomy for essential blepharospasm. Digital Journal of Ophthalmology : DJO /, 23(4), 8-12.
[4] Wabbels B, Roggenkamper P. Long-term follow-up of patients with frontalis sling operation in the treatment of essential blepharospasm unresponsive to botulinum toxin therapy. Graefes Arch Clin Exp Ophthalmol 2007;245(1):45-50.
[5] Bansal, S., & Das, S. (2017). Frontalis sling surgery: A treatment modality for cyclic oculomotor nerve palsy. Saudi Journal of Ophthalmology : Official Journal of the Saudi Ophthalmological Society., 31(3), 196-198.
[6] Sanghera M, Grossman RG, Kalhorn CG et al. Basal ganglia neuronal discharge in primary and secondary dystonia in patients undergoing pallidotomy. Neurosurgery 2003;52:1358–73.
[7] Eltahawy HA, Saint-Cyr J, Giladi N et al. Primary dystonia is more responsive than secondary dystonia to pallidal interventions:outcome after pallidotomy or pallidal deep brain stimulation. Neurosurgery 2004;54(3):613–9.
[8] Bronte-Stewart H. Surgical therapy for dystonia. Curr Neurol Neurosci Rep 2003;3(4):296-305.
[9] Yoshor D, Hamilton WJ, Ondo W et al. Comparison of thalamotomy and pallidotomy for the treatment of dystonia. Neurosurgery 2001;48:818–824.
[10] Gunduz, A., Foote, K., & Okun, M. (2017). Reengineering deep brain stimulation for movement disorders: Emerging technologies. Curr Opin Biomed Eng, 4, 97-105
[11] Vidailhet M, Vercueil L, Houeto JL et al. Bilateral deep-brain stimulation of the globus pallidus in primary generalized dystonia. N Engl J Med 2005;352:459–67.
[12] Marceglia, S., Rosa, M., Servello, D., Porta, M., Barbieri, S., Moro, E., & Priori, A. (2017). Adaptive Deep Brain Stimulation (aDBS) for Tourette Syndrome. Brain Sciences., 8(1), Brain sciences. , 2017, Vol.8(1).
[13] Arlotti, M., Marceglia, S., Foffani, G., Volkmann, J., Lozano, A., Moro, E.,Gogiamanan F, Prenassi M, Bocci T., Cortese, F., Rampini, P. Barbieri, S., Priori, A. (2018). Eight-hours adaptive deep brain stimulation in patients with Parkinson disease. Neurology.,Neurology. , 2018.

