Older Adults and Oral Conditions
The proportion of older adult people in developed countries has increased considerably during the last few decades and is expected to increase further in the next years. This is a result of what has been called the “demographic transition,” a term used to describe the increasing life expectancy and concurrent fall in the birth rate occurring in industrialized nations [1].
Japan has led the way in this shift with people aged 65 years or more currently compromising 23% of the Japanese population and projected to increase to 38% of the population by 2050 [2]. Although this growth in the percentage of elderly in the population may not be as marked in other developed countries, the same trends are evident.
In China, the equivalent estimates are 8% currently with 23% being projected for 2050; in Europe, the equivalent proportions are 16% and 27%; in North America, 13% and 22% and in New Zealand, 14% and 25%.
This demographic shift to greater percentages of older adults will have important implications for health care services. Larger populations of elderly often mean greater numbers of the oldest of the old: that is, people 80 years of age and older, who frequently are frailer and face more morbidity and disabilities. Consequently, an increasing proportion of health care services will be required for these individuals than is routinely needed for younger elderly, the 65–79 year olds [3].
Advances in oral health care and treatment during the past few decades have resulted in a reduced number of edentulous adults with the proportion of adults who retain their teeth until late in life increasing substantially [2], [4].
Like what you’re learning? Download a brochure for our Geriatric Dentistry Master Program certificate or master’s degree program.
The numbers of older people with oral related problems, including those who are dentate has also increased. The complexity of oral health status, numerous co-existing systemic diseases and the use of multiple medications make older people more vulnerable to oral problems when compared to younger groups. This is even truer for those elders who are cognitively impaired [5], [6].
Recent literature has described the relevant medical characteristics of old age, including the multi-morbidity, polypharmacy, frailty, disability and care dependency as the “geriatric syndrome” [7]. Van der Putten and de Baat suggested that weakened oral health has the potential to become a component of the geriatric syndrome [8].
Epidemiology of Oral Conditions Among Older Patients
The oral health of older people has warranted considerable research attention in the last two to three decades. In discussing the epidemiology of oral conditions among this group, Murray included the following listing of findings:
- Tooth loss
- Dental caries
- Periodontitis
- Dry mouth
- Oral pre-cancerous or cancerous lesions
- Oral health related quality of life [9]
Van der Putten and de Baat added to this list the findings of substantial tooth wear, oral implants and sophisticated tooth and implant supported removable dentures and/or fixed dental prostheses [8], concluding that older adults are in continuous need of preventive and curative oral health care.
Mulligan and Vanderlinde suggested a model to follow in order to cover the interactions of the medical, behavioral, dental/oral and psychosocial factors of older adults [10].
All of these topics in any detail would result in a lengthy treatise beyond the scope of most periodicals. Therefore, this paper will limit itself to a discussion of just one of the clinical conditions frequently seen in older adults: dry mouth.
We feel this topic to be particularly relevant as a geriatric dentistry foundation topic, for in caring for elders, practitioners soon discover the interrelationship of many of the oral conditions previously mentioned with dry mouth. Therefore this review article will focus on diminished salivary flow, or dry mouth sensations from a clinical and symptomatic perspective. Causes, treatment and prevention will be considered.
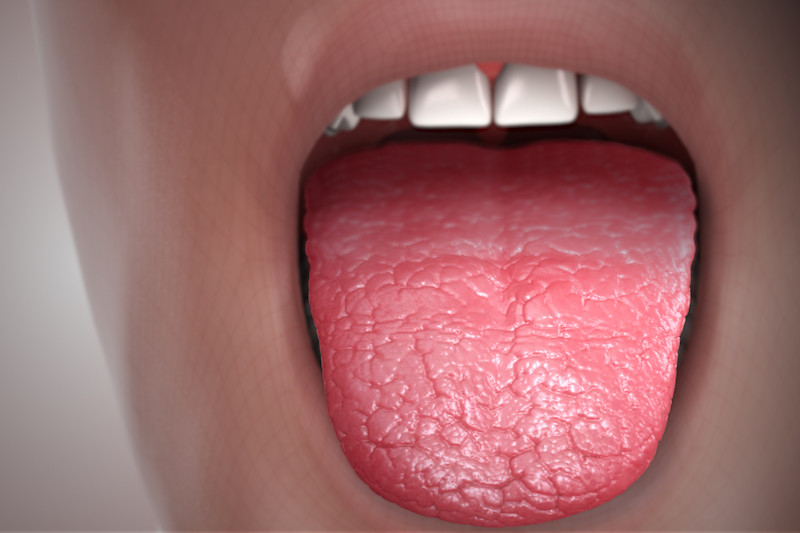
Dry Mouth in Older Adult Patients
When it comes to treatment of dry mouth conditions, either objective or subjective, there are no easy answers as to the best course of action for a specific individual.
There are many conditions that can cause dry mouth. While most of the cited studies have examined the most difficult cases of dry mouth, that is, those that are a result of treatment for head and neck cancer, there are many individuals who demonstrate dry mouth from far less grievous circumstances.
Taking a thorough history in an attempt to discover the contributor to and/or cause of the signs and/or symptoms and based on those findings, attempting to select the most appropriate intervention is the critical role of the practitioner.
Additional factors such as patient comfort, motivation, access to the various treatments, and cost will also play a role in the selection of a successful therapy.
It is important to recall that water is an essential component for life [11]. Begin by educating the patient about possible causes of dry mouth. An analysis of fluid intake (e.g. a daily fluid diary) may be a good place to start and may also be the most practical, cost effective and efficient treatment with the best risk-benefit ratio.
Postgraduate Geriatric Dentistry
Are you looking for improved ways to diagnose, treat, and manage the oral healthcare of older patients? Explore our online master’s and certificate program in Geriatric Dentistry.

