Dystonic reactions consist of involuntary, tonic contractions of skeletal muscles. [2] [3] [4]
Akathisia reactions occur as a subjective experience of motor restlessness. [5] Patients may complain of an inability to sit or stand still, or a compulsion to pace or cross and uncross their legs.
Parkinsonian reactions manifest themselves as tremor, rigidity, and akinesia, which shows as a slowness in initiating motor tasks and fatigue when performing activities requiring repetitive movements (bradykinesia).
Like what you’re learning? Test your diagnosis skills with USC’s Virtual Patient Simulation. Review real-life patient histories, conduct medical interviews and exams, make a diagnosis, and create a treatment plan for patients experiencing orofacial pain.

Proposed Mechanism
When a medication or drug induces a dystonic extrapyramidal syndrome (EPS) reaction, it typically involves the muscles of the head, face and jaw producing spasm, grimacing, tics, or trismus. Most of the literature has focused on the more severe acute dystonic EPS reactions which occur with use of antipsychotic medications. [6]
In addition to the antipsychotics, several antiemetics with dopamine receptor blocking properties have also been associated with tardive dystonia. [7] These include prochlorperazine, promethazine and metoclopramide. Of course, milder reactions do occur which vary in intensity and even wax and wane over time. The most commonly reported offending agents that are not neuroleptics are the selective serotonin reuptake inhibitors (SSRI) and the stimulant medications and illegal drugs.
Selective Serotonin Reuptake Inhibitors
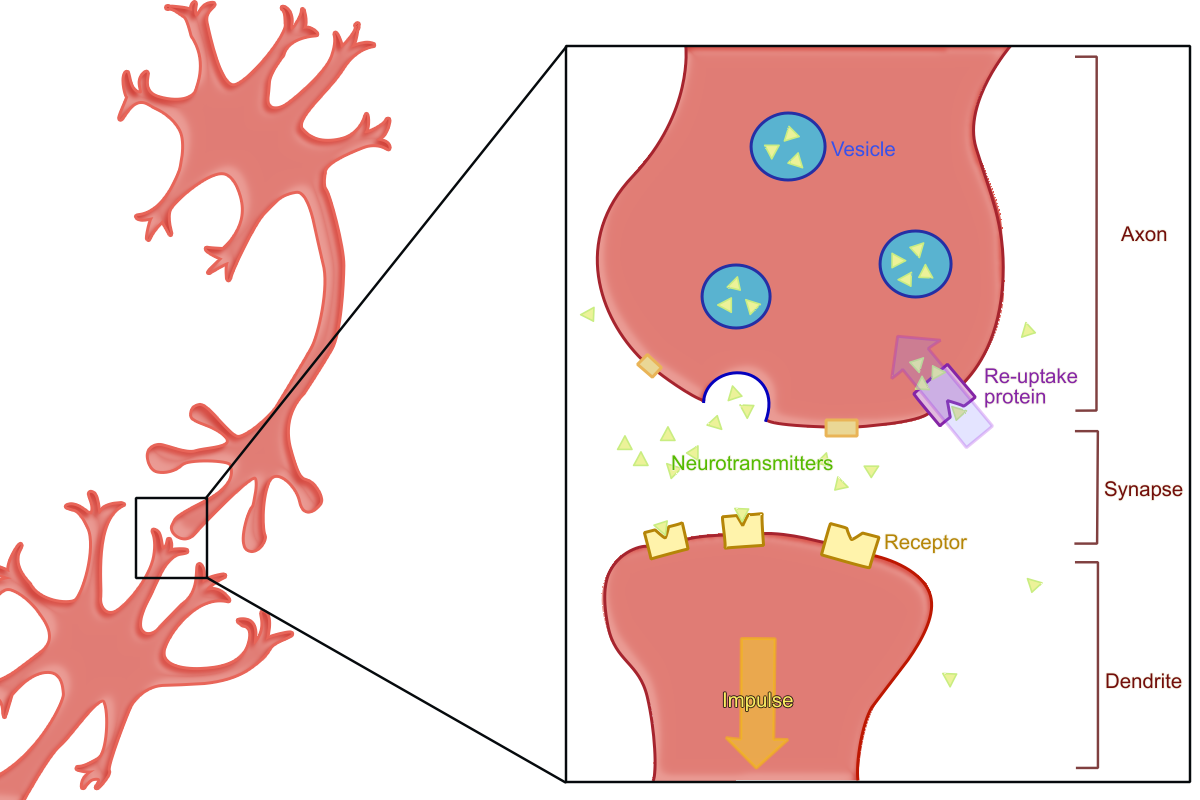
Selective serotonin reuptake inhibitors (e.g. fluoxetine, fluvoamine, paroxetine, sertraline, citalopram, escitalopram) are used for depression and a variety of other mental illness. Unforturnately these drugs are reported to produce increased clenching and bruxism as a side effect. [8]
Actually the term SSRI-induced bruxism may not be accurate in that the actual motor behavior does not present as brief strong sleep-state-related contractions as seen in bruxism but more of an increased sustained non-specific activation of the jaw and tongue musculature.
Patients generally describe an elevated headache and tightness in their jaw, tongue and facial stucutures and the best information available about the effect of SSRI class medications on oromandibular structures comes from a study in 1999, which examined the acute effects of paroxetine on genioglossus activity in obstructive sleep apnea. [9]
They found that 40mg of paroxetine produced a clear augmentation of peak inspiratory genioglossus activity during NREM sleep. Only case-based literature exists at this time and further polysomnographic studies on the motor effects of SSRI’s are necessary in order to define prevalence, risk factors and establish a causal relationship between SSRI use and oral motor disorders.
Illegal Drugs
Illegal drugs such as methamphetamine, cocaine, 3,4-methylenedioxymethamphetamine (Ecstasy) [10] and various legal prescription stimulants such as methylphenidate, phentermine, pemoline, dextroamphetamine, amphetamines, and diethylproprion have all been reported to induce bruxism and dystonic extrapyramidal reactions. [11] [12] [13] [14]
All stimulant drugs have the potential to cause extrapyramidal reactions and they are being used in greater numbers to treat obesity and or as stimulants for children with attention deficit hyperactivity disorder (ADHD) or narcolepsy and even for severe depression. [15]
Treatment
Removing the potential motor activating medications is the first step of treatment when a suspected drug-related motor disorder is present. [16] Both amantadine (SymmetrelT M) 200-400 mg/d po [17] and benzodiazepines have been shown to be effective for recurrent neuroleptic-induced dystonic reactions. [18]
Some patients with SSRI-induced dystonic EPS experience relief with a reduction in the dose of SSRI or the other stimulant drug e.g. fluoxetine (ProzacT M) changed from 20 mg/day to 10 mg/day.
Other patients respond to the addition of buspirone (BusparT M) in doses of 5-15 mg per day. [19] [20] Buspirone appears to be an effective treatment based on a few case reports. This drug may have an additional benefit of relieving anxiety that may be a co-existing condition. It is usually well tolerated and carries a low risk of significant side effects.
Finally, switching to antidepressants that have not yet been associated with inducing bruxism such as the mirtazapine (RemeronT M) or nefazodone (SerzoneT M) is an option.
Earn an Online Postgraduate Degree in Orofacial Pain and Oral Medicine
Do you want to deliver appropriate and safe care to your growing and aging dental patients? Consider enrolling in our online, competency-based certificate or master’s program in Orofacial Pain and Oral Medicine.

References
[1] Fernandez HH, Friedman JH. Classification and treatment of tardive syndromes.
Neurologist. 2003 Jan;9(1):16-27
[2] Chouinard G. New nomenclature for drug-induced movement disorders including tardive dyskinesia.
J Clin Psychiatry. 2004;65 Suppl 9:9-15.
[3] Trosch RM. Neuroleptic-induced movement disorders: deconstructing extrapyramidal symptoms.
J Am Geriatr Soc. 2004 Dec;52(12 Suppl):S266-71.
[4] Tarsy D, Baldessarini RJ, Tarazi FI. Effects of newer antipsychotics on extrapyramidal function.
CNS Drugs. 2002;16(1):23-45.
[5] Inada, T. (2017). [Drug-Induced Akathisia].
Brain Nerve, 69(12), 1417-1424.
[6] Caroff, S., Ungvari, G., & Cunningham Owens, D. (2018). Historical perspectives on tardive dyskinesia.
Journal of the Neurological Sciences., Journal of the neurological sciences.
[7] Wijemanne, S., Jankovic, J., & Evans, R. (2016). Movement Disorders From the Use of Metoclopramide and Other Antiemetics in the Treatment of Migraine.
Headache : The Journal of Head and Face Pain., 56(1), 153-161.
[8] Beers, E., & Van Grootheest, A. (2007). [Bruxism as a side effect of serotonin re-uptake inhibitors].
Ned Tijdschr Tandheelkd, 114(9), 388-390.
[9] Berry RB, Yamaura EM, Gill K, Reist C. Acute effects of paroxetine on genioglossus activity in obstructive sleep apnea.
Sleep. 1999 Dec 15;22(8):1087-92.
[10] Baylen CA, Rosenberg H. A review of the acute subjective effects of MDMA/ecstasy.
Addiction. 2006 Jul;101(7):933-47.
[11] Grau-López, L., Daigre, C., Mercado, N., Casas, M., & Roncero, C. (2017). Dystonia in Methylphenidate Withdrawal: A Case Report.
Journal of Addiction Medicine., 11(2), 154-156.
[12] Matthew, B., & Gedzior, J. (2015). Drug-induced parkinsonism following chronic methamphetamine use by a patient on haloperidol decanoate.
The International Journal of Psychiatry in Medicine., 50(4), 405-411.
[13] See SJ, Tan EK. Severe amphethamine-induced bruxism: treatment with botulinum toxin.
Acta Neurol Scand. 2003 Feb;107(2):161-3.
[14] Winocur E, Gavish A, Voikovitch M, Emodi-Perlman A, Eli I. Drugs and bruxism: a critical review.
J Orofac Pain. 2003 Spring;17(2):99-111.
[15] Malki GA, Zawawi KH, Melis M, Hughes CV. Prevalence of bruxism in children receiving treatment for attention deficit hyperactivity disorder: a pilot study.
J Clin Pediatr Dent. 2004 Fall;29(1):63-7.
[16] Bressman SB. Dystonia update. Clin Neuropharmacol. 2000 Sep-Oct;23(5):239-51.
[17] Niemann, N., & Jankovic, J. (2018). Treatment of Tardive Dyskinesia: A General Overview with Focus on the Vesicular Monoamine Transporter 2 Inhibitors.
Drugs., Drugs. , 2018.
[18] Nanda, S., Sawhney, C., & Sinha, C. (2013). In response to: Midazolam-induced acute dystonia reversed by diazepam.
Journal of Anaesthesiology Clinical Pharmacology., 29(2), 268-269.
[19] Sabuncuoglu, O., Ekinci, O., & Berkem, M. (2009). Fluoxetine-induced sleep bruxism in an adolescent treated with buspirone: A case report. Special Care in Dentistry Official Publication of the American Association of Hospital Dentists, the Academy of Dentistry for the Handicapped, and the American Society for Geriatric Dentistry., 29(5), 215-217.
[20] Pavlovic ZM. Buspirone to improve compliance in venlafaxine-induced movement disorder.
Int J Neuropsychopharmacol. 20:1-2, 2004.

